Oximetry FAQs | NOVA Pulmonary (Northern Virginia)
What is oximetry?
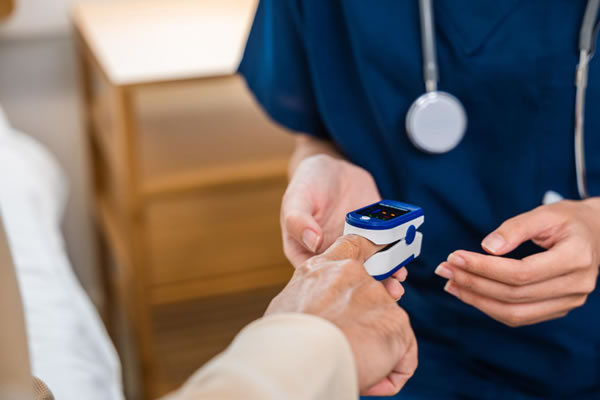
Oximetry is a quick, non-invasive way to measure the oxygen level in your blood using a small device called a pulse oximeter, typically placed on your fingertip.
What is pulse oximetry used for?
Pulse oximetry helps evaluate and monitor oxygen levels in people with lung and heart conditions, including Chronic Obstructive Pulmonary Disease, Asthma, and Pneumonia. It’s also used during routine exams, sleep studies, and exercise testing.
What is a normal oxygen level?
A normal oxygen saturation (SpO₂) level is typically between 95% and 100% for healthy individuals. Your provider will interpret results based on your overall health and medical history.
What is considered low oxygen (hypoxia)?
Low oxygen levels, known as Hypoxia, are generally below 90%. This may require medical evaluation and treatment.
How does a pulse oximeter work?
A pulse oximeter uses light beams passed through your finger to estimate how much oxygen your red blood cells are carrying.
Is oximetry painful?
No, oximetry is completely painless and non-invasive. It does not involve needles or blood draws.
How long does an oximetry test take?
A spot check takes just a few seconds to a minute. Continuous monitoring may be used over longer periods, such as overnight.
Can oximetry be done at home?
Yes, many patients use home pulse oximeters to monitor oxygen levels, especially those with chronic lung conditions or recovering from illness.
When should I use a pulse oximeter at home?
You may be advised to use one if you have:
- Chronic lung disease
- Shortness of breath
- Recent respiratory infection
- Oxygen therapy needs
Follow your provider’s guidance on when and how often to check your levels.
What factors can affect oximetry readings?
Several factors can impact accuracy, including:
- Cold hands or poor circulation
- Nail polish or artificial nails
- Movement during the test
- Skin pigmentation variations
- Improper device placement
Can oximetry diagnose lung disease?
Oximetry does not diagnose specific conditions, but it helps detect low oxygen levels and monitor diseases like Chronic Obstructive Pulmonary Disease and Pulmonary Fibrosis.
When should I seek medical attention based on oximetry readings?
You should contact a healthcare provider if:
- Your oxygen level drops below 90%
- You experience worsening shortness of breath
- You have symptoms like chest pain or confusion
Is oximetry used during sleep studies?
Yes, oximetry is commonly used during sleep evaluations to monitor oxygen levels and detect breathing-related sleep disorders.
Office Locations
Conveniently located near you in Dulles, Leesburg, (Loudoun County) and Vienna, (Fairfax County), VA
NOVA Pulmonary – Dulles
24430 Stone Springs Boulevard
Suite 550
Dulles, VA 20166
NOVA Pulmonary – Lansdowne
19415 Deerfield Avenue
Suite 301
Landsdowne, VA 20176
Meet the team at NOVA Pulmonary Critical Care and Sleep Associates
Dr. Aditya N Dubey, M.D, F.C.C.P. – Founder
Specialty:
Pulmonary, Critical Care and Sleep Medicine
Board Certified by American Board of Internal Medicine in the Subspecialities of Pulmonary Medicine, Critical Care Medicine and Sleep Medicine. Learn more about Dr. Dubey
Dr. Petra Thomas, M.D.
Specialty:
Pulmonary Medicine
Board Certified by American Board of Internal Medicine in the Subspecialities of Pulmonary Medicine. Learn more about Dr. Thomas
Dr. Arman Murabia, M.D.
Specialty:
Pulmonary, Critical Care and Sleep Medicine
Board Certified by American Board of Internal Medicine in the Subspecialities of Pulmonary Medicine, Critical Care Medicine and Sleep Medicine. Learn more about Dr. Murabia

Dr. Zara Martirosyan, MD
Specialty:
Sleep Medicine & Internal Medicine Specialist
Board-certified physician in both Sleep medicine and Internal medicine. Learn more about Dr. Martirosyan
Rebekah Lee, AGNP-C, Lead APP
Nurse Practitioner. Learn more about Rebekah Lee
Paulos Abebe PA-C
Physician Assistant Learn more about Paulos Abebe PA-C

Katie Cameron, PA
Physician Assistant Learn more about Katie Cameron, PA-C
Christine Amorosi, AGNP-C
Nurse Practitioner. Learn more about Christine Amorosie
Pulmonary Testing
Pulmonary Function Test

Lung Volume Test

Cardiopulmonary Exercise Test (CPET)

Chest X-ray/CT Scan